Type 2 diabetes is often introduced as a lifelong condition, something you “manage” forever with medications, restrictions, and constant monitoring. But over the last decade, that narrative has begun to change.
Clinicians, researchers, and metabolic health experts are now asking a more precise question: Can Type 2 diabetes be reversed (not cured, but driven into remission) by correcting the underlying metabolic dysfunction?
The answer, based on current scientific understanding, is YES, for many people, under the right conditions.
This blog breaks down the biology, the evidence, and the real‑world practicality of Type 2 diabetes reversal, without hype, shortcuts, or oversimplification.
First, What Actually Is Type 2 Diabetes?
Type 2 diabetes is not primarily a blood sugar disease.
Type 2 diabetes is not primarily a blood sugar disease.
It is a metabolic condition rooted in insulin resistance, where:
- Cells (especially in muscle, liver, and fat tissue) stop responding efficiently to insulin
- The pancreas compensates by producing more insulin
- Over time, pancreatic beta cells fatigue and insulin secretion declines
- Blood glucose rises as a downstream effect
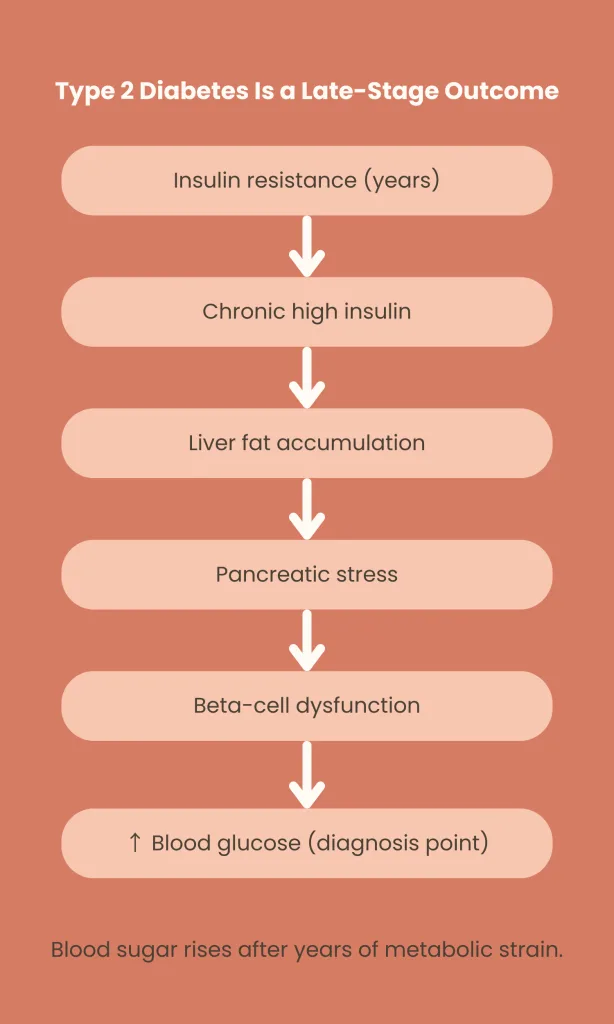
By the time fasting glucose or HbA1c crosses diagnostic thresholds, insulin resistance has often been developing silently for years.
This distinction is important, because treating blood sugar alone does not address the root cause.
Reversal vs Cure: An Important Clarification
Let’s define terms clearly.
- Cure would mean the disease can never return, regardless of lifestyle or physiology
- Remission (Reversal) means blood glucose remains in the non‑diabetic range without medication, as long as metabolic health is maintained
Type 2 diabetes can go into remission, but the underlying susceptibility may remain.
Think of it like putting a fire out by removing fuel, not deleting the possibility of fire forever.
The Core Mechanism Behind Reversal: Insulin Sensitivity
Every credible diabetes reversal strategy, regardless of dietary philosophy, converges on one goal: Improving insulin sensitivity and reducing metabolic overload
Key biological shifts seen in remission include:
- Reduced liver fat → improved fasting glucose control
- Reduced pancreatic fat → restoration of beta‑cell responsiveness
- Improved muscle glucose uptake
- Lower chronic insulin levels
- Reduced systemic inflammation
When these processes reverse, blood glucose normalizes as a consequence, not as the primary target.
What Does the Research Consistently Show?
Across different populations and intervention models, remission has been observed through:
- Significant and sustained weight loss (reduction in visceral and ectopic fat)
- Calorie reduction with metabolic restructuring
- Improved diet quality and glycaemic control
- Increased physical activity (especially resistance training)
- Early intervention after diagnosis
Importantly, remission is more likely when:
- Diabetes duration is shorter
- Beta‑cell function is not severely impaired
- Lifestyle changes are structured and supported
This reinforces one critical insight:
Type 2 diabetes progression is biologically modifiable.
Is Weight Loss the Only Way?
Weight loss plays a powerful role but it is not the full story.
Some individuals improve glycaemic control significantly without dramatic weight loss, particularly when:
- Ectopic fat (liver and pancreatic fat) is reduced
- Diet quality improves (fiber, protein, micronutrients)
- Meal timing and insulin demand are optimized
- Muscle mass increases
In other words:
Metabolic health is about where fat is stored, how insulin behaves, and how cells respond, not just the number on the scale.
The Role of Nutrition: Beyond “Sugar Control”
Effective nutritional strategies for remission focus on:
- Lowering glycaemic load, not eliminating carbohydrates indiscriminately
- Prioritising fiber‑rich, whole‑food carbohydrate sources
- Adequate protein to preserve muscle mass and metabolic rate
- Healthy fats that support insulin signalling and reduce inflammation
- Micronutrients that support insulin signalling (magnesium, zinc, chromium)
Rigid extremes often fail long‑term.
Sustainable remission comes from metabolic literacy, not food fear.
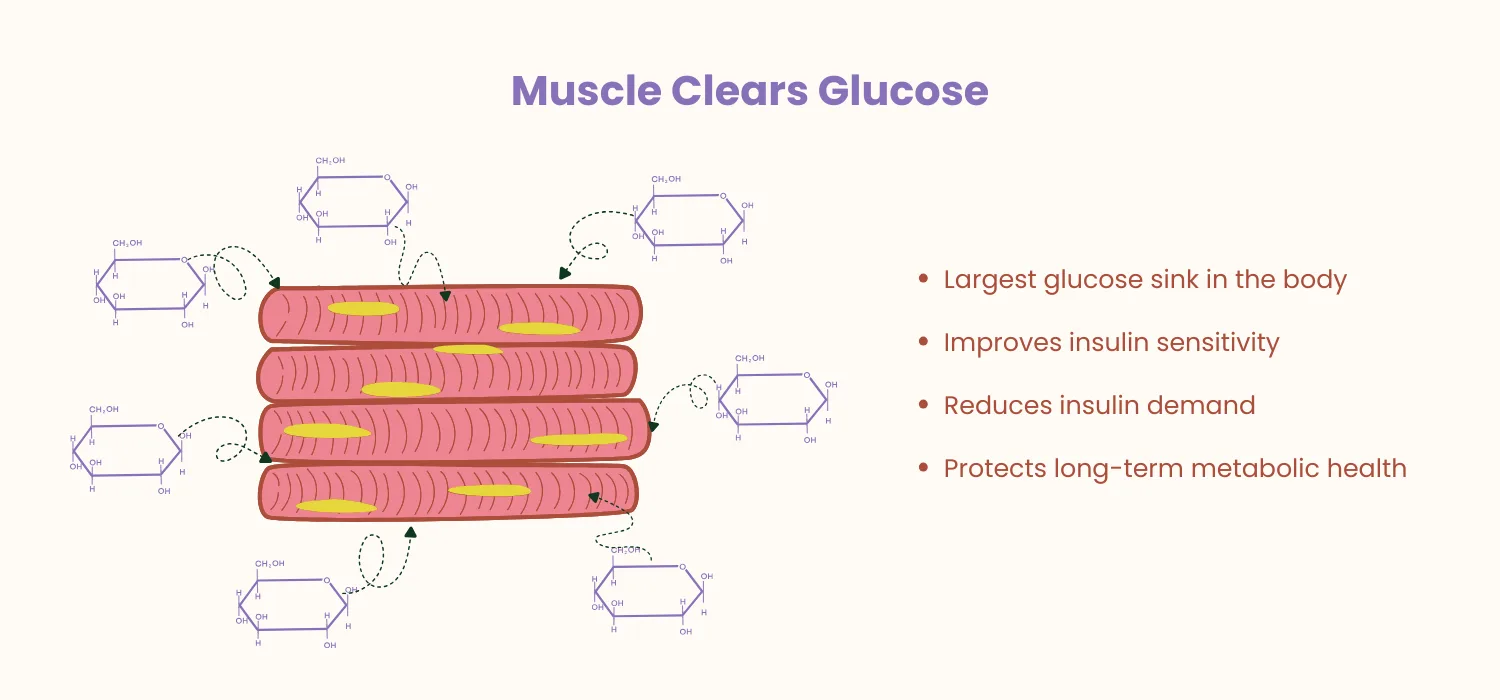
Exercise: The Most Underused Insulin‑Sensitiser
Muscle is the largest glucose‑disposal organ in the body.
Regular physical activity:
- Increases insulin‑independent glucose uptake
- Improves mitochondrial efficiency
- Reduces visceral fat
- Enhances insulin receptor sensitivity
Resistance training is particularly powerful, underutilised and often under‑prescribed compared to walking alone.
What About Medications?
Medications are not a failure.
They can:
- Reduce glucose toxicity
- Protect beta‑cell function
- Provide metabolic breathing room
In many remission journeys, medications are used temporarily alongside targeted nutrition and lifestyle interventions.
Who Is Most Likely to Achieve Remission?
While every individual is different, remission is more achievable when:
- Diagnosis is relatively recent
- HbA1c is moderately elevated
- There is residual insulin production
- Interventions are personalised and structured
- Sleep, stress, and hormonal health are addressed
This is why early, informed intervention matters more than motivation alone.
Why Many People Are Told It’s “Not Reversible”
Historically, diabetes care focused on:
- Glucose control over insulin resistance
- Medication escalation over metabolic repair
- Short consultations over behavioural restructuring
The medical system evolved around control, not reversal.
That paradigm is changing but slowly.
A More Accurate Question to Ask
Instead of:
“Is Type 2 diabetes reversible?”
A better question is:
“How reversible is my metabolic dysfunction and what will it take to restore insulin sensitivity?”
That answer is personal, measurable, and actionable.
The Takeaway
Type 2 diabetes is not simply a lifelong sentence.
It is a metabolically driven condition that can enter remission when the underlying physiology is addressed.
Reversal is not quick.
It is not linear.
And it is not achieved through hacks.
But with the right strategy, education, and support, normal glycaemic control without medication is a realistic outcome for many.
And even when full remission is not achieved, every step toward improved insulin sensitivity meaningfully reduces complications and improves quality of life.
A personalised, physiology-driven approach can make the difference between temporary control and long-term metabolic stability.
If you’re navigating insulin resistance or Type 2 diabetes and are tired of trial-and-error advice, book a consultation with Dt. Ishita Singhal.

0 Comments